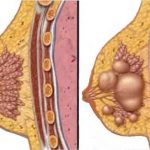
Breast cancer is the second most common cancer in women. Mammography is very common test for breast screening programs – it is actually X-ray of the breast (two X-ray pictures of each breast). This screening tool is used for breast cancer detection and precise diagnosis. It is well known that thanks to mammography breast cancer can be discovered at very early stages which is very important for successful treatment and high survival rates (up to 98-100%).
Usually screening mammograms is not recommended before 40 (especially if woman does not have any risk factors and/or breast abnormalities). Age factor is very important for mammogram. As women breasts are dense before 40, the diagnostic ability of this method is not 100% as in dense breasts sometimes cancerous transformations are not visible. Modern machines with 3-D technologies (digital mammogram) can discover breast cancer even in very dense breasts. Digital mammogram is performed in the same way as a traditional test, but the image is viewed on a computer monitor with options to enlarge or target different zones, all images can be stored as a digital file and can be printed on film.
Screening mammograms can detect breast cancers in very earliest stages (even “in-situ”) – dramatically reducing mortality rates (especially in women between 40 and 69). Screening mammograms can also find microcalcifications (tiny deposits of calcium) that sometimes indicate the presence of breast cancer.
Unfortunately breast cancer in girls is also becoming a new problem for oncologists and for families with cancer history. This is why scientists are working on modern tools for breast cancer early diagnosis and treatment.
Mammography procedure
It is simple routine test to check for breast cancer or other breast abnormalities (lumps, cysts, etc.). Duration of the procedure is about 15-20 minutes. Mammograms require very small doses of radiation and the risk of radiation exposure from a mammogram is considered virtually nonexistent. Only repeated X-rays can have the influence at body cells.
Best time for screening mammogram is one week after the menstrual period – when breasts are least likely to be tender.
Health provider will place each breast between special plates. The breast is compressed as flat as possible between the film holder and a rectangle of plastic (so called “paddle”) which presses down onto the breast from above. The compression should only last few seconds – just enough to take the X-ray picture. The only unpleasant feeling could be from compression and squeezing of the breast, but it is necessary for better pictures and detailed images.
If you have breast lump or cyst or implant, doctor should be informed in advance.
Mammogram results
Results could be positive, negative, false positive and false negative.
Positive test means breast tumor was noted on the mammogram.
Negative test means both breast are healthy without any abnormalities.
False-positive test means X-ray picture looks abnormal with certain signs similar to cancer – actually showing not existing breast cancer. In these cases additional diagnostic test are needed including digital mammography, ultrasound, biopsy or MRI (Magnetic resonance imaging).
False-positive mammogram could trigger stress, anxiety, depression and useless panic. In addition, women could spend money for additional medical consultations and tests.
False-negative results occur when mammogram appears normal but actually woman already has breast cancer at early stages. Some breast cancers do not show up on mammograms and could be hidden in dense breast tissue. The main cause of false-negative results is high breast density.
According to medical experts, overall, screening mammograms miss about 10-15% of breast cancers that are present at the time of screening. False-negative results can be noted in younger women with dense breasts. As a woman ages, her breasts usually become more fatty and false-negative results become less likely. Unfortunately false-negative results of mammogram could lead to later diagnosis and later treatment which could reduce the survival rates.