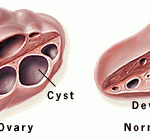
Symptoms of the Polycystic Ovarian Syndrome (PCOS) tend to start gradually. Often, hormone changes that lead to PCOS start in the early teens, after the first menstrual period. Symptoms could be more noticeable after weight gain in puberty. Usually women with PCOS grow many small cysts on their ovaries – that is why it is called polycystic ovarian syndrome. The cysts are not harmful but lead to hormone imbalances.
PCOS means a complex of symptoms, consisting of some combination of the following symptoms that vary with each individual. All PCOS possible symptoms include:
- Multiple ovarian “cysts” (12 or more) – in most cases the size of “cysts” is 2-9mm but often cysts vary between 5mm and 15mm;
- Increased (2-5 times) volume of ovaries (thanks to multiple “cysts”) – enlarged ovaries (> 10 cubic centimeters) on both sides;
- Oligimenorrhea (rare periods) or amenorrhea (absence of periods);
- Anovulation – cycles without ovulation – not ovulating, or releasing a mature egg from the ovary each month;
- Infertility;
- Acne and oily skin;
- Obesity (different stages) or inability to lose weight;
- Hirsutism (abnormal excessive hair grow on face and body);
- Hair loss similar to male pattern baldness and/or Thinning of scalp hair;
- Insulin resistance and possibly diabetes;
- Acanthosis nigricans – patches of dark, thickened, velvety skin behind the neck, on the thighs, or on the vulva – this is usually a sign of insulin resistance;
- High blood pressure;
- Impaired lung function;
- Sleep apnea;
- Fatty liver degeneration (NAFLD);
- Disordered immune system;
- Mood disorders, including anxiety and depression;
- Appetite disorder;
- High blood fats (cholesterol and triglycerides);
- Increased probability of cardiovascular disease or diabetes;
- Multiple hormone imbalances (androgens, cortisol, estrogens, progesterone, LH, FSH, insulin, prolactin and thyroid hormones).
Some girls and women with PCOS could have just few symptoms but some could have a big list of symptoms. It is not known why different persons have different number of symptoms during PCOS.
The most common alarming PCOS symptoms which bring girls and women to doctor usually include:
![]() Menstrual problems – infrequent, irregular or absent periods which could be heavy when they do arrive;
Menstrual problems – infrequent, irregular or absent periods which could be heavy when they do arrive;
![]() Hirsutism (male-type hair growth on face and body);
Hirsutism (male-type hair growth on face and body);
![]() Weight gain or upper body obesity.
Weight gain or upper body obesity.
PCOS & Oligomenorrhea
In healthy women usually at the beginnings of the menstrual cycle ovaries start to develop 20 eggs every month – these eggs mature in little sacs called “cysts”. Over the course of the month, one egg will become dominant and draw most of the hormones being produced, eventually being released by the ovary to be fertilized or shed with the period. During PCOS women fail to produce the correct balance of estrogen necessary to help one egg become dominant. As a result, all 20 eggs develop but remain as “cysts” which in turn results in the production of androgens (male hormones) and reduced production of progesterone.
Because of androgens and decreased level of progesterone, women with PCOS usually develop irregular periods, fail to ovulate (anovulation), or fail to have a period at all (called “amenorrhea”). When a period does occur, many women with PCOS note that their bleeding can be quite heavy.
During PCOS women could have less than nine menstrual cycles in a year (more than 35 days between cycles) to no menstrual periods.
PCOS & Hirsutism
One of the common symptoms of PCOS is hirsutism – excess hair growth on face and body or loss of hair. The main reason for the change in hair growth is increased level of androgens (male hormones produced by polycystic ovaries).
Androgens are a group of hormones, such as testosterone, found at high levels in men but present in women at much lower levels. PCOS sufferers, though, often have higher than normal levels of androgens. These excess hormones can cause a disorder known as hirsutism. Women with hirsutism typically have thicker and darker hair growing on their face and body. The areas most commonly affected are the mustache and beard, though the extra hair growth may also be noticed on the chest, back, stomach, arms, legs, and pubic region. While not all women with PCOS will have hirsutism, a whopping 95% of those women with hirsutism will have PCOS. Ferriman-Gallway Hirsute Score is the most objective for hair grow estimation.
Thinning of the hair can also occur in women with PCOS and some may experience male-pattern baldness. This type of hair loss is known as “androgenic alopecia.” Although alopecia is a disorder that results in complete hair loss, the type of alopecia that affects PCOS sufferers is caused by an increase in androgen levels.
PCOS & Infertility
Main reason for infertility in PCOS women is anovulation – absence of ovulation. Given that period disruption with PCOS is due to irregular or absent ovulation, it is not surprising that it is a common cause of infertility. It is not usually 100% absolute, and some women with PCOS will ovulate normally, some will ovulate less frequently (leading to a delay to pregnancy) and some will not ovulate at all, meaning that for some infertility treatment, likely fertility drugs such as Clomid, will definitely be necessary.
Women who have already been diagnosed with PCOS may not be too surprised by their fertility problems. However, a number of women may not even realize that they have PCOS until they start trying to conceive. While 75% of women with PCOS do have menstrual problems, 25% do not. In these women, perhaps they have always had regular periods but never realized that they were not ovulating. Others may have had the occasional irregular period, but felt that it was nothing to be too concerned about, assuming a skipped period was due to stress or some other factor. Regardless of the reason, some women will only learn of their PCOS condition when they are investigated for infertility problems.
Infertility is not present in every case of PCOS. However, persistent anovulation is frequently seen in PCOS despite menstruation. This is known as an anovulatory cycle. Ovulation does occur intermittently thereby allowing for pregnancy although it often takes longer to conceive. In a minority of cases, women with PCOS are infertile.
PCOS & skin issues
High androgen levels are also the reason why various skin conditions can develop in women with PCOS. Perhaps the most common are acne, which usually develops on the face, particularly along the jaw line, and on the chest and back, and oily skin. The hormone dihydrotestosterone, or DHT, is thought to be responsible, as it tends to stimulate the oil glands, resulting in a greater production of oil, which can clog the pores and cause acne.
Other skin problems noted by PCOS sufferers are skin tags and darkening of the skin. Skin tags are often located around the armpit area, along the bra line or on the neck. These thick lumps of skin can be removed quite easily, though, by a dermatologist. If you notice the skin around your neck, underarms, groin or skin folds getting darker and thicker, you may have Acanthosis Nigricans. This darkening is a symptom of insulin resistance, which is thought to be one of the main causes of PCOS nowadays.
PCOS & Obesity
This is a double-edged sword for women with PCOS, around 40% of sufferers being overweight. Obesity itself will initiate the symptoms described above in some women who would not have otherwise suffered had they remained of normal weight. It will worsen the symptoms for those who do have PCOS and, unfortunately, the hormone changes associated with PCOS make weight loss more difficult. But is this excess weight gain due to androgens or insulin resistance?
It is somewhat difficult to say just what causes the obesity. High androgen levels can make it difficult to lose weight as can insulin resistance. And while insulin resistance contributes to obesity by promoting fat storage, obesity itself contributes to insulin resistance, which in turn exacerbates PCOS symptoms.
PCOS & Insulin resistance
During some cases of PCOS body does not respond as well to insulin, the primary hormone which helps the body use and deal with glucose or sugar. This causes elevated blood glucose levels and is a major risk factor for Type 2 Diabetes – prolonged exposure to high levels of glucose and the reduced sensitivity of body cells to insulin eventually make the body unable to deal with sugar. When glucose levels are persistently high, complications develop. These include problems with eye sight, kidney disease, and neuropathy, which is a loss of feeling and circulation in the body limbs.
Impaired glucose tolerance or diabetes mellitus (sugar diabetes) is often seen as a result of insulin resistance and these signs and symptoms may also be present.
PCOS & Hormonal dysfunctions
Multiple hormone imbalances is pretty typical for PCOS. In general several hormones are involved in so called “PCOS hormonal chaos” – Androgens (testosterone), Cortisol, Estrogens, LH (luteinizing hormone), FSH (follicle stimulating hormone), Insulin, Progesterone, Prolactin and Thyroid hormones.
PCOS occurs when there are high levels of androgens in the body, often as a result of an excess of LH (luteinizing hormone). An associated decrease in FSH (follicle-stimulating hormone) affects the way the body deals with these androgens. The estrogen levels are subsequently reduced while the androgen levels are elevated. This affects the menstrual cycle and ovulation. These differences in the hormone levels will present with a host of features affecting multiple systems of the body.
Usually most PCOS clients are recommended to have hormonal tests and the following is most typical for PCOS:
- Luteinizing hormone (LH) – high levels of luteinizing hormone in the blood;
- Prolactin – high levels of prolactin in the blood (hyperprolactinemia);
- Androgens – high levels of free testosterone or free androgen index;
- Glucose – high levels of blood glucose (hyperglycemia);
- Insulin – high levels of insulin (hyperinsulinemia due to insulin resistance);
- Cholesterol – high levels of blood cholesterol (hypercholesterolemia).
(information used from – http://www.ovarian-cysts-pcos.com/pcos.html & http://www.womens-health.co.uk/pcos1.asp)